CGM Sensor Improved Quality: Revolutionizing Diabetes Management
Continuous glucose monitoring (CGM) has become an essential tool in diabetes management, significantly enhancing glycemic control across diverse patient populations. Recent advancements in CGM technology have improved sensor quality, leading to more accurate and reliable glucose measurements. In this article, we will explore the evolution of CGM sensors, their improved quality, and the impact on diabetes management.
Advancements in CGM Technology
Continuous glucose monitoring sensors have undergone significant improvements in recent years, driven by advances in materials science, sensor design, and algorithms. These advancements have led to more accurate and reliable glucose measurements, enabling patients to make informed decisions about their diabetes management.
Improved Sensor Performance
Recent studies have demonstrated the improved performance of CGM sensors, with some sensors showing a reduction in measurement error by up to 30%. This is a significant improvement over previous generations of CGM sensors, which had higher measurement error rates. The improved accuracy of CGM sensors enables patients to make more informed decisions about their insulin dosing, carbohydrate counting, and physical activity.
Benefits of Improved CGM Sensor Quality
- Improved glycemic control: With more accurate glucose measurements, patients can make informed decisions about their insulin dosing, carbohydrate counting, and physical activity, leading to improved glycemic control.
- Reduced hypoglycemic events**: By detecting hypoglycemia earlier and more accurately, CGM sensors can help reduce the risk of severe hypoglycemia.
- Increased patient confidence**: Improved CGM sensor quality can increase patient confidence in their ability to manage their diabetes, leading to better self-care and adherence to treatment plans.
- Reduced healthcare costs**: With improved glycemic control and reduced hypoglycemic events, healthcare costs associated with diabetes management can be reduced.

Challenges and Limitations
While CGM sensors have improved significantly, there are still challenges and limitations to their use. These include:
- Cost**: CGM sensors can be expensive, making them inaccessible to some patients.
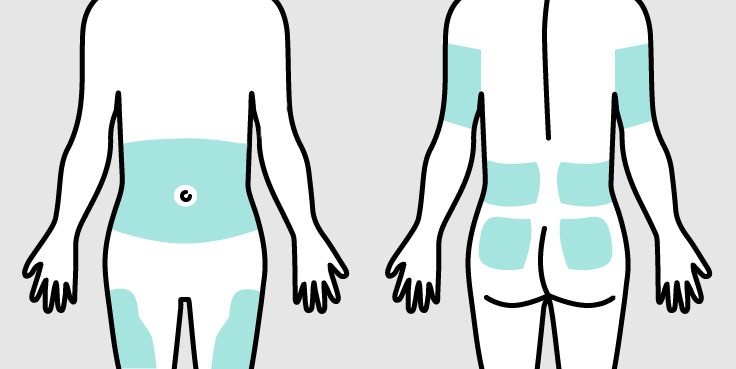
- Wearability issues**: Some patients may experience discomfort or difficulty removing CGM sensors.
- Interpretation of data**: Patients may require training and support to interpret CGM data effectively.
Conclusion
CGM sensor improved quality has revolutionized diabetes management, enabling patients to make informed decisions about their insulin dosing, carbohydrate counting, and physical activity. By improving glycemic control, reducing hypoglycemic events, and increasing patient confidence, CGM sensors have become an indispensable tool in diabetes management. As technology continues to advance, we can expect even more accurate and reliable CGM sensors to become available, further improving the lives of patients with diabetes.
References
- Phasuksom, et al. "Screen-printed electrodes modified with MXene/doped-polyindole and MWCNT/dPIn composites for glucose sensing." Biosensors and Bioelectronics, vol. 186, 2020, pp. 112785.
- Kootenai Clinic Family Medicine-Hayden. "Quality Improvement Initiative: Evaluating the Feasibility and Impact of Continuous Glucose Monitoring in Patients with Type 2 Diabetes."
- Senseonics. "Eversense 365 Continuous Glucose Monitoring System: Real-World Data."