Unraveling the Psychology Behind GLP-1 Treatment: A Comprehensive Review
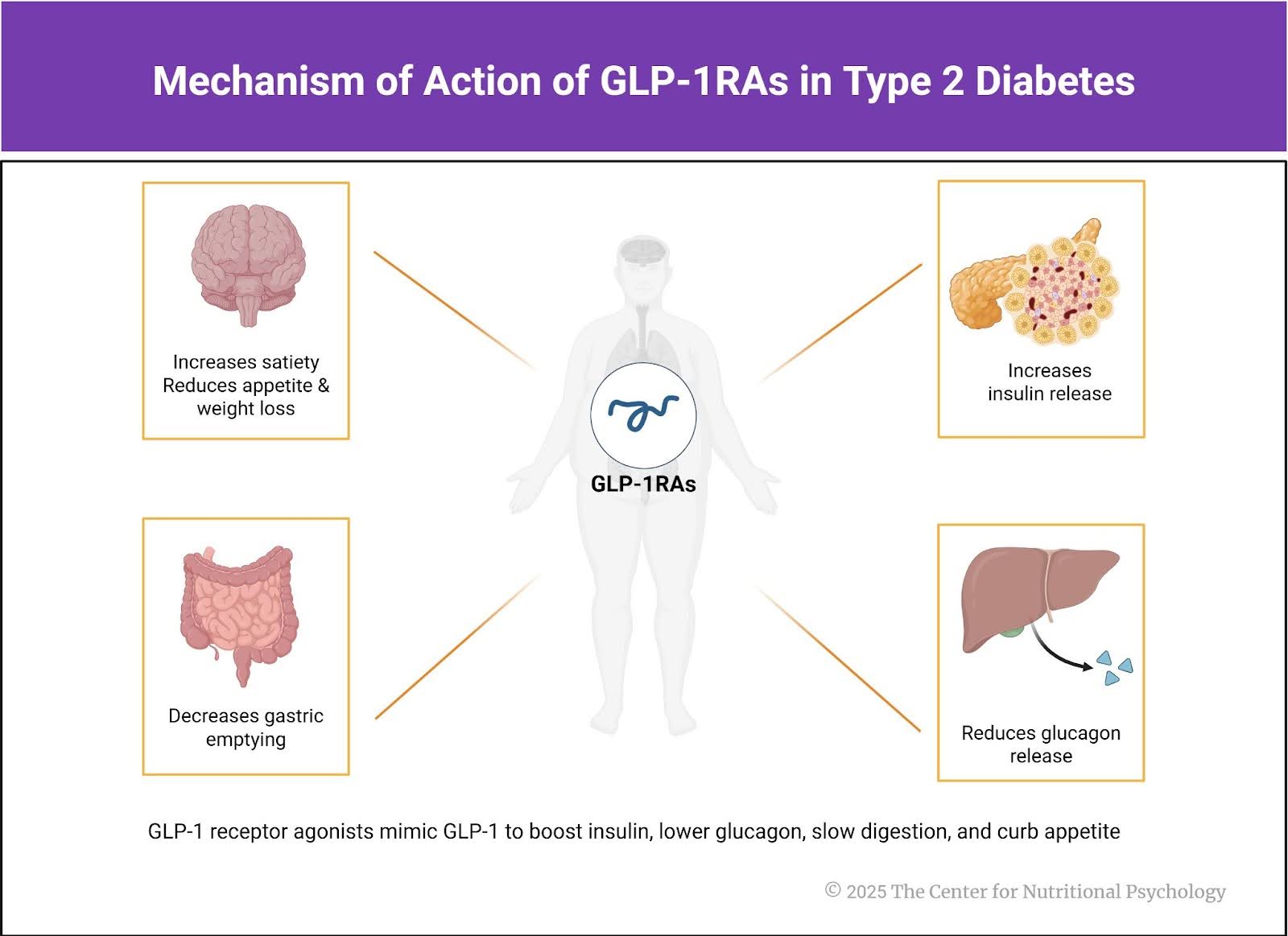
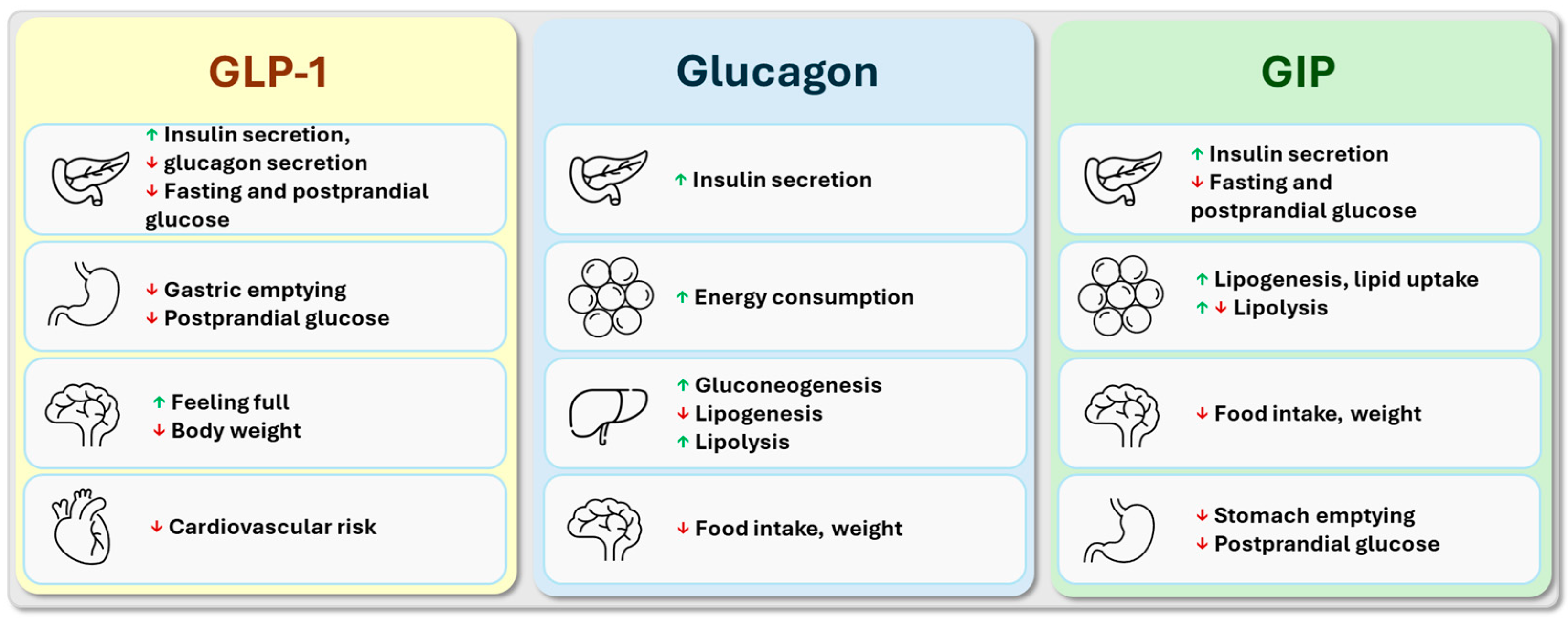
Glucagon-like peptide-1 receptor agonists (GLP-1RAs) have emerged as a promising treatment option for managing type 2 diabetes mellitus and obesity. However, the psychological implications of these medications have been a topic of increasing interest in recent years. In this article, we will delve into the current literature on the psychological dimensions of GLP-1 treatment, exploring its potential benefits and drawbacks.
Psychological Treatment and GLP-1: A Complex Relationship
Research suggests that GLP-1 treatments can have a profound impact on mental health, with studies indicating a 42% lower risk of worsening mental illness in individuals with depression and anxiety. The exact mechanism behind this effect is still unclear, but it is believed to involve the modulation of the brain's reward system and the reduction of inflammation.
Improved mood and emotional regulation
Reduced cravings and substance use disorders
Enhanced motivation and goal-directed behavior
Increased feelings of self-efficacy and self-esteem
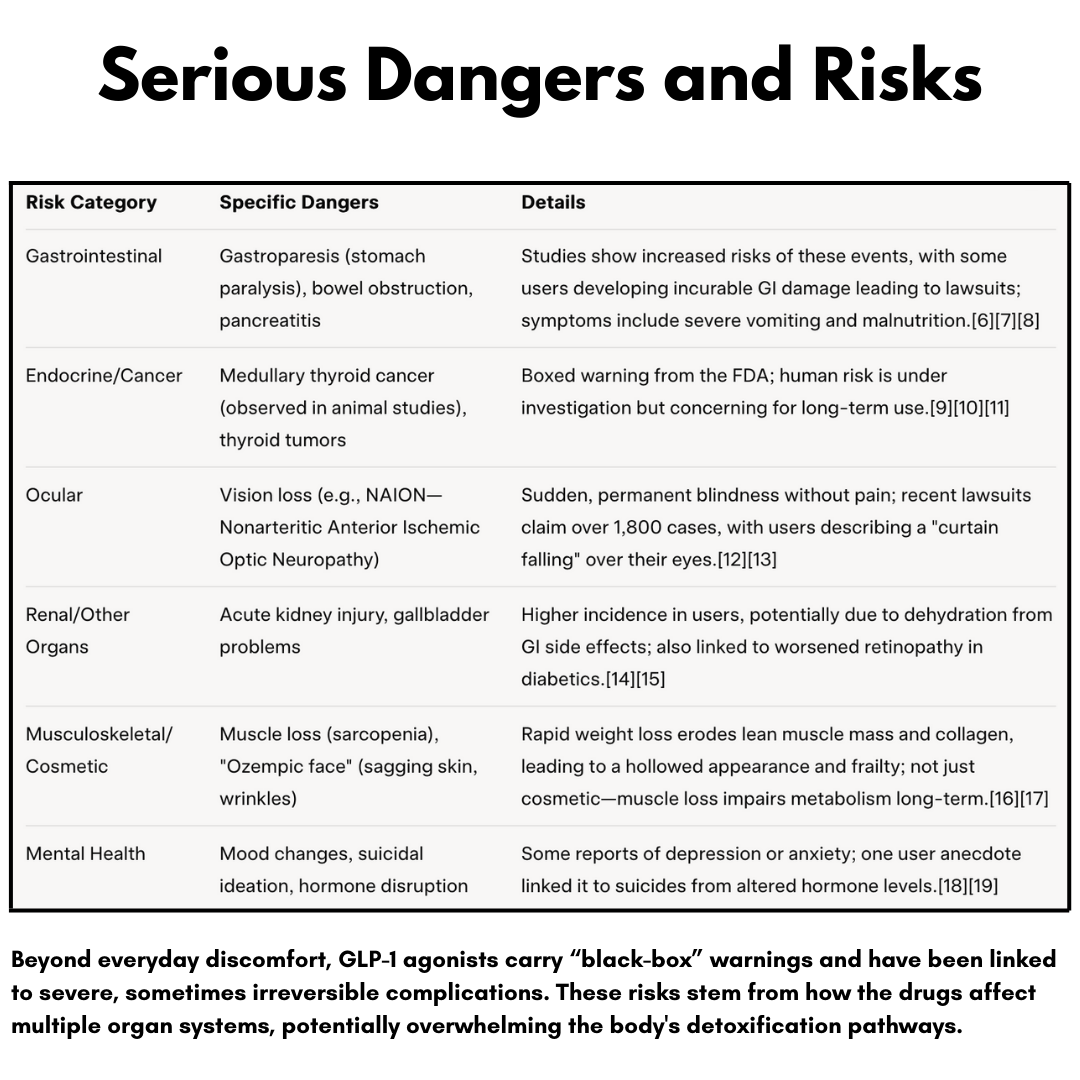
The Dark Side of GLP-1: Misuse and Eating Disorders
While GLP-1 treatments have shown promise in addressing mental health concerns, they also carry a risk of misuse and eating disorders. A study found that a whopping 22% of patients developed nutritional deficiencies within 12 months of starting GLP-1 treatment. Furthermore, experts warn that GLP-1 medications can trigger eating disorder relapse by mimicking symptoms and disrupting intuitive eating signals.

What Happens When You Stop GLP-1 Treatment?
When patients discontinue GLP-1 medications, their body undergoes several physiological changes that contribute to weight regain. GLP-1 receptor activity returns to baseline within 1-2 weeks of stopping medication, leading to a loss of the artificial enhancement of satiety and weight loss benefits.
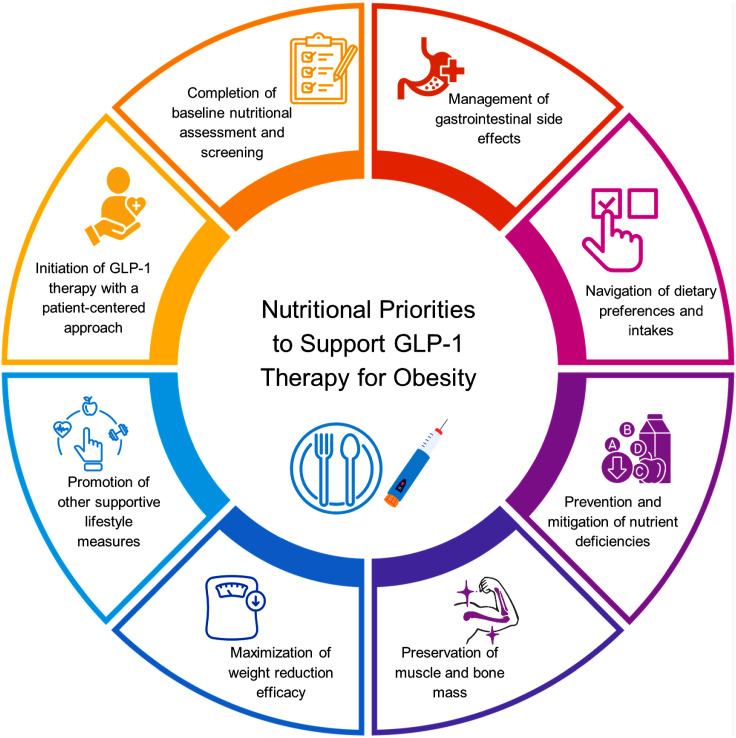
The Role of Psychology in GLP-1 Treatment
To maximize the benefits of GLP-1 treatment, it is essential to incorporate psychological interventions into the treatment plan. This can include cognitive-behavioral therapy (CBT), interpersonal psychotherapy (IPT), and self-help techniques. By addressing the psychological dimensions of weight loss, patients can develop healthier behaviors and manage the emotional challenges associated with rapid transformation.
Conclusion
GLP-1 treatments offer a promising new frontier in the treatment of obesity and mental health concerns. However, their psychological implications are complex and multifaceted. By understanding the potential benefits and drawbacks of GLP-1 treatment, healthcare professionals can provide more comprehensive care to patients and optimize treatment outcomes. Ultimately, a holistic approach that incorporates psychological interventions and monitoring is essential for maximizing the benefits of GLP-1 treatment.