GLP-1 Drug Effects on Pancreatic Islet Cells: A Comprehensive Review
The glucagon-like peptide-1 (GLP-1) receptor agonists have revolutionized the treatment of type 2 diabetes mellitus (T2DM) by improving glycemic control, reducing body weight, and lowering blood pressure. GLP-1, a proglucagon derivative, is secreted by gut L-cells in response to meals and enhances glucose-induced insulin secretion from pancreatic islet β-cells. This incretin effect accounts for as much as half of the postprandial insulin response, making GLP-1 an attractive antidiabetic drug candidate.
GLP-1 Mechanism of Action
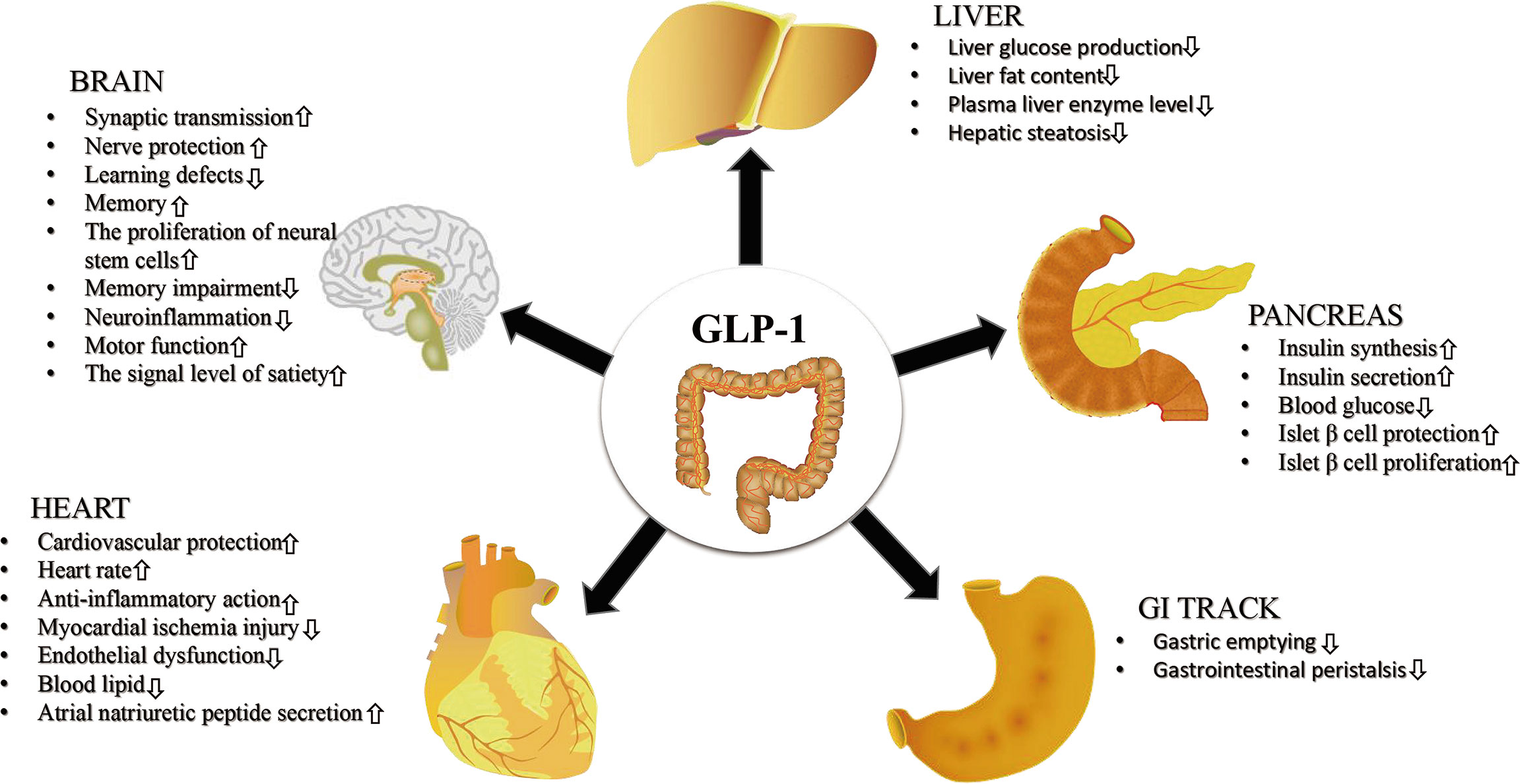
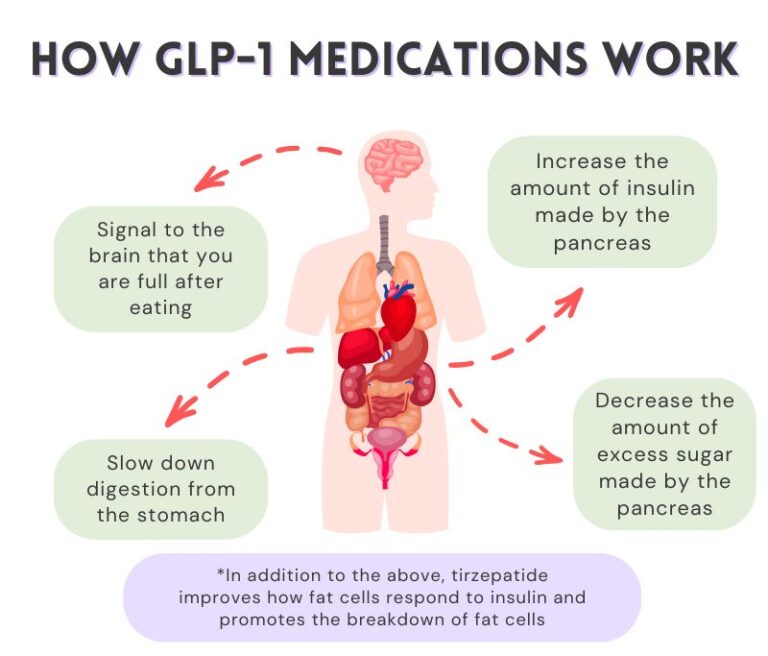
GLP-1 exerts its effects on pancreatic islet cells through several mechanisms. It stimulates glucose-stimulated insulin secretion and protects β-cells, while its extrapancreatic effects include cardioprotection, reduction of hepatic glucose production, and regulation of satiety. The rapid degradation of GLP-1 by dipeptidyl peptidase 4 (DPP-4) raises questions about how its effects are mediated on target organs such as pancreatic β-cells.
Alternative Pathways for GLP-1 Effects
Several alternative pathways have been proposed for the incretin effect on pancreatic islet cells. These involve L-cell-derived GLP-1 via neuronal activation and α-cell-derived GLP-1 via auto/paracrine mechanisms. The α-cells in the pancreatic islets produce glucagon, which is a major regulator of glucose metabolism. GLP-1 has been shown to modulate the activity of α-cells, leading to reduced glucagon secretion and improved glucose control.
GLP-1 Receptor Activation and Insulin Secretion
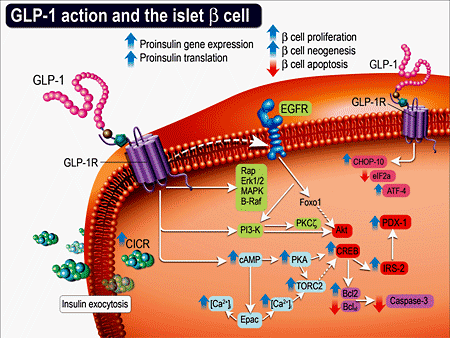
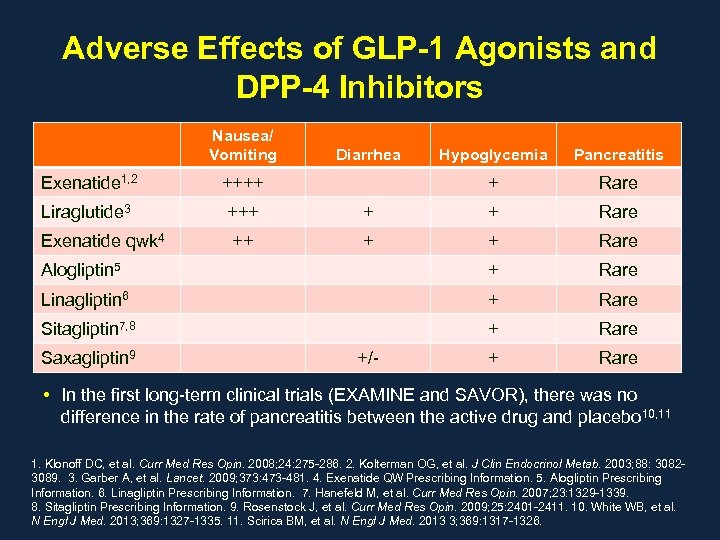
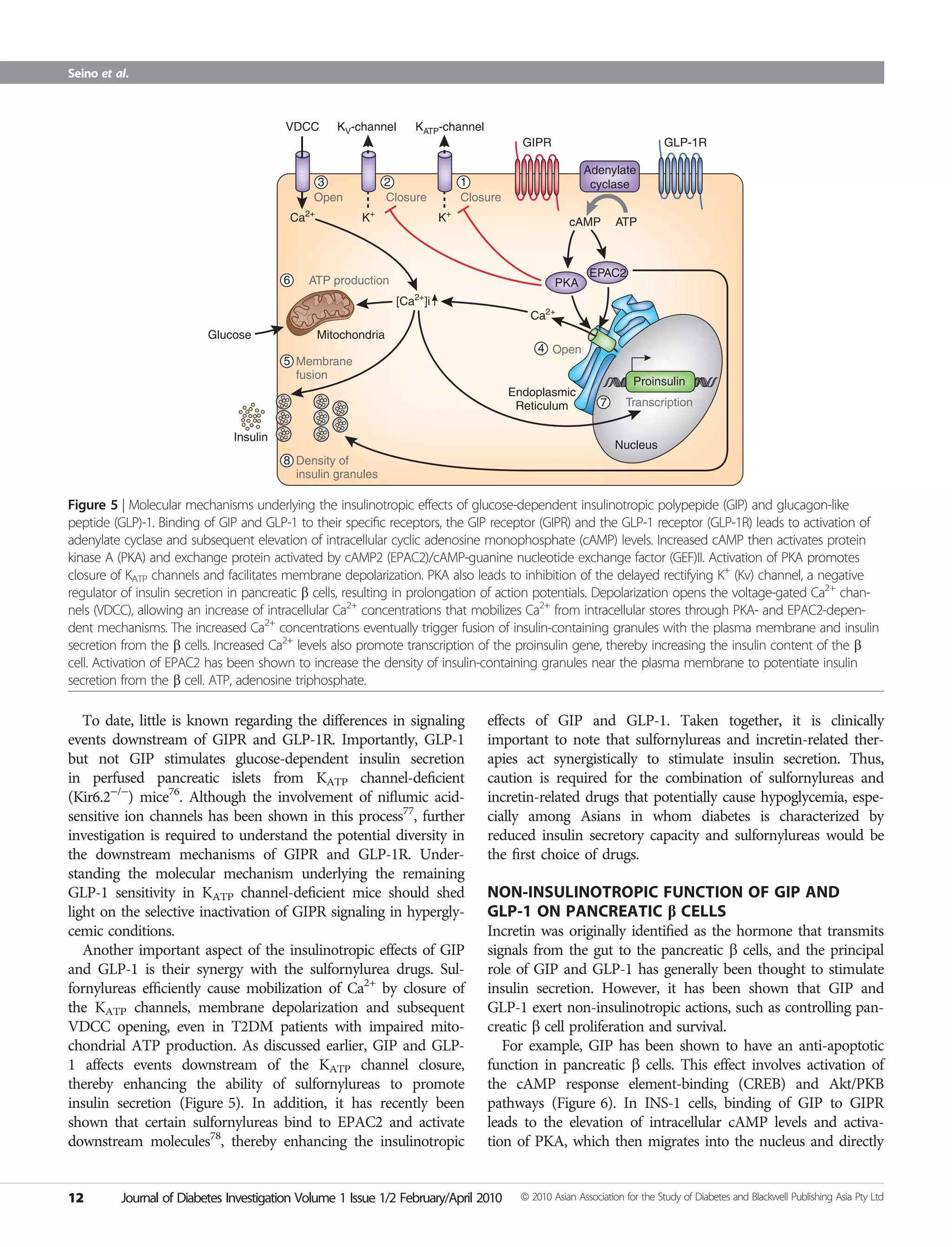
GLP-1 receptor activation stimulates insulin secretion from β-cells in the islets of Langerhans in response to rising plasma glucose levels. This glucose-dependent mechanism explains the low risk of hypoglycemia with GLP-1 receptor agonists. The intracellular signaling pathways involved in GLP-1 receptor activation include cAMP-dependent protein kinase (PKA), phosphatidylinositol 3-kinase (PI3K), and protein kinase B (Akt).
GLP-1 and Pancreatic Islet Cell Function
GLP-1 has been shown to have beneficial effects on pancreatic islet cell function, including improved insulin secretion, enhanced insulin sensitivity, and reduced β-cell apoptosis. The effects of GLP-1 on pancreatic islet cell function are mediated through its receptors, which are expressed on β-cells, α-cells, and other cell types in the islets.

GLP-1 and Weight Loss
GLP-1 receptor agonists, such as liraglutide and semaglutide, have been shown to promote weight loss in individuals with T2DM. The mechanisms underlying GLP-1-induced weight loss are complex and involve multiple pathways, including reduced hunger, increased satiety, and improved glucose metabolism.
Conclusion
GLP-1 receptor agonists have revolutionized the treatment of T2DM by improving glycemic control, reducing body weight, and lowering blood pressure. The effects of GLP-1 on pancreatic islet cell function are complex and involve multiple pathways, including enhanced insulin secretion, improved insulin sensitivity, and reduced β-cell apoptosis. Further research is needed to fully understand the mechanisms underlying the effects of GLP-1 on pancreatic islet cell function and to develop new GLP-1-based therapies for the treatment of T2DM.
References
[1] Drucker, D. J. (2013). The biology of incretin hormones. Cell Metabolism, 17(6), 931-946.
[2] Holst, J. J. (2007). The physiology of glucagon-like peptide 1. Physiological Reviews, 87(4), 1409-1439.
[3] Ahren, B. (2009). GLP-1: A novel therapeutic approach to diabetes treatment. Journal of Clinical Endocrinology and Metabolism, 94(11), 4321-4331.
[4] Yang, H. et al. (2018). GLP-1 receptor agonists and cardiovascular risk: A systematic review and meta-analysis. Journal of the American College of Cardiology, 71(10), 1153-1163.